Benign Prostatic Hyperplasia, better known as BPH, is a enlargement of the prostate gland (non-cancerous) due to an over development of prostate cells. The gland is a critical component of the male reproductive system.
The prostate gland secretes a fluid into the urethra during the ejaculation process. The prostate gland is located below the neck of the urinary bladder, encompassing the urethra. Although there is no consensus on the cause of BPH many experts believe it is caused due a decrease in testosterone as a man ages.
Nearly 50% of men at age 50 will have Benign Prostatic Hyperplasia, and by the time reach 80 years of age, there is an 80-90% chance of developing an enlarged prostate. In the US, more then 2 million men are treated annually for BPH. While symptoms of BPH and prostate cancer are similar, Benign Prostatic Hyperplasia has never been proven to be a precursor in developing prostate cancer.
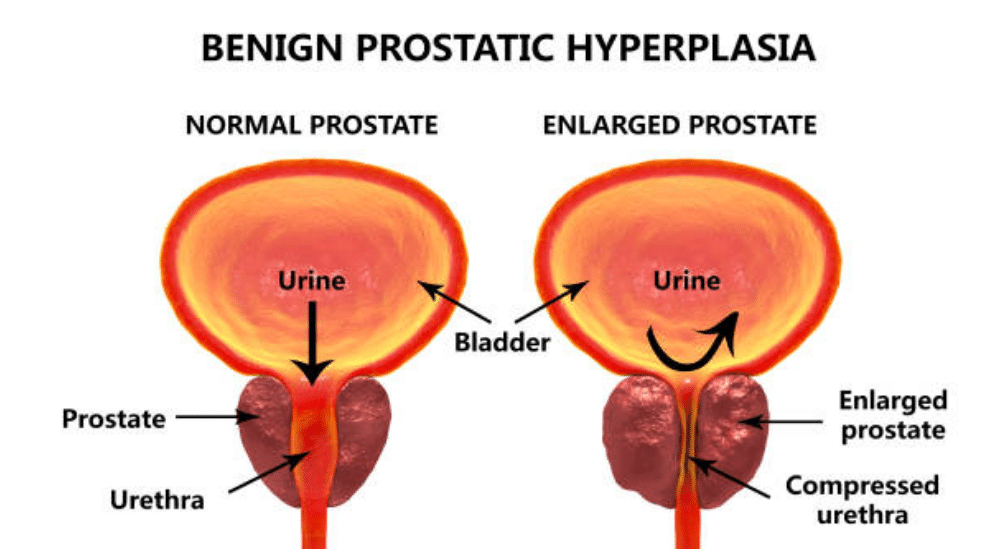
As the prostate becomes enlarged, it squeezes the urethra which runs directly through the center of the gland and as time progresses it can restrict urine flow. At first, the symptoms of BPH are mild and tolerable. As the condition becomes more severe, the symptoms can affect a man’s quality of life.
The most common Symptoms of BPH are:
- Urinating frequently at night
- An urgency to urinate often
- Urinary flow doesn’t start right away
- Urinary flow is intermittent, it stops and goes
- The slow flow of urine
- finding blood in the urine
- A Feeling the bladder isn’t empty
- Pain or burning sensation during or after urinating
- Impotence
- Having pain during orgasms
With such symptoms, finding a restroom influences where one can go. Having to excuse oneself frequently and being uncomfortable a great deal of the time can be annoying if not embarrassing in social environments. At a certain point, it becomes necessary to see a urologist like Dr. Razdan, a medical expert specializing in diseases of the urinary and genital area. Once he confirms the diagnosis of BPH, he will recommend a treatment option. There is no cure for BPH so the main goal of the treatment is to find relief.
The cause of benign prostatic hyperplasia is not clear
Though their is much research on BPH, the root cause of benign prostatic hyperplasia has yet to be identified. Their are two main factors that stand out to help predict this condition:
- family history of BPH
- age
Many experts tend to agree that BPH results from a decrease in testosterone as men get older. Some of the other theories include Estrogen and the presence of DHT. Due to the large population of men who suffer from BPH, ongoing research is being conducted to identify the true cause and the least invasive methods to treat the disease.
Treatment options for BPH can vary from drug therapy to surgery
For most men with benign prostatic hyperplasia, the prostate will continue to grow until medical intervention becomes necessary. With the help of a world renowned urologist like Dr. Razdan, each man can develop the appropriate and best treatment plan with which they are both comfortable. Some of the options currently available will be found below.
Watch and Wait Option:
For very mild symptoms with no decrease in a man’s quality of life, sensitivity to drugs, or when surgery is not an option, this approach can be desirable. With regular follow-ups, Dr. Razdan will monitor the progress of the disease and the symptoms. This is normally a temporary option because the prostate will continue to grow with time, and more advanced treatment will become required. Additionally, advanced treatment will become recommended irregardless of the level of discomfort due to the possibility of harming the urogenital region. Over time, the wall of the bladder will thicken and the muscles weaken to the point that the bladder can not completely empty itself. This may result in repetitive urinary tract infections, urine retention, painful bladder stones, and damage to organs in the urinary and reproductive areas. Eventually if these conditions continue, a man’s urine may back up to the kidneys, creating the potential for painful kidney stones and renal disease.
Medication Therapy:
There are 3 groups of Medications:
- Medications that relax the muscles of the prostate and lower bladder allowing the urethra to open
- Medications which shrink the growth of the prostate
- Medications which increase bladder capacity.
Some names of these drugs are: Flomax, Proscar, Cardura and, Avodart. When prescribed this medication, it must be taken for the remainder of the man’s life. These medications can be very effective, however the downside is their side-effects which include sexual functioning issues. For some patients this option is unacceptable.
Surgical Interventions:
Their are several surgical options available. The procedures discussed below are the most efficient and effective of all treatment options currently available today.
Years ago, BPH was surgically treated by an operation known as an Open Prostatectomy. This is a major procedure where a large incision on the abdomen is made. This surgery is performed in a hospital under general anesthesia. The Urologist will make an incision on the patient’s abdomen and either (resect) remove the gland or cuts off (transect) the overgrowth. After the surgery, the patient leaves the surgical operating room with two catheters which will remain in the patient for up to one week. This procedure requires a long-term rehabilitation period and can be painful. Today, a prostatectomy is only performed when the patient’s prostate has grown too large to be removed laparoscopically or robotically, additionally if there are bladder stones present, or when the bladder needs to be repaired.
TURP better known as (Transurethral Resection of the Prostate) is the more commonly performed procedure. This procedure is done in a hospital or out-patient surgical facility also using general anesthesia, or under conscious sedation. Using a special imaging scope known as a resectoscope, the Urologist enters the urethra through the penis and cuts away pieces of the overgrown prostate gland using electricity. At the end of the procedure, a urinary catheter is placed in the patient and is removed the next day. This procedure takes under 2 hours and the patient can be discharged in 1-2 days. The patient can usually return to daily activities in 4 weeks, however strenuous activity may take many months. The benefit of this procedure is its safety and effectiveness in opening the urinary route. Possible side-effects directly after the procedure include uncomfortable and occasional difficulty urinating and blood in the urine. There is a possibility of long-term recovery issues, including impotence and retrograde ejaculation. TURP is considered to be the optimum treatment for BPH today.
Minimally Invasive, Non-Surgical Treatments:
There are several Minimally invasive treatments including Lasers, microwaves, radio frequency waves, and ultrasound. These energy forms can be directed at the prostate by entering the urethra with a cystoscope or similar instrument. The effectiveness of using focused energy is positive for the short term with discharge on the same day, less discomfort urinating, and a quicker return to daily activities than with surgery. Many of these Minimally invasive treatments have little data and needs further study before a comparison can be made between non-surgical and surgical treatment options.






